National Medical Support Orders
By Karen Hooper | Published May 5, 2017
Best practices for support orders when the employee is not currently enrolled in coverage
We just received a National Medical Support Order.
Q 1. Who is responsible for completing the form?
Q 2. Since the employee did not elect coverage, what date are we using to enroll him per this order?
Compliance Team Answer:
Q 1. As the plan administrator, the employer is responsible for completing the National Medical Support Order.
Q 2. The employee should be enrolled as soon as possible and generally no later than the first of the month following receipt/review of the order.
Here’s a more complete explanation:
A National Medical Support Notice (NMSN), is similar to a Qualified Medical Child Support Order (QMCSO) and essentially has the same effect.
Mandatory Enrollment of Employee and Child
The plan is required to enroll both the employee and the child in this case—even if the employee doesn’t want to be enrolled. There is no election procedure for the employee here. Assuming the employee and child are eligible, the plan must complete the enrollment of the child (and employee if not previously enrolled) regardless of whether the employee does not wish to enroll him/herself or the child.
Note that sometimes that can get contentious because it’s the only time the employer must force an employee to enroll and pay for his or her own (and the child’s) coverage. However, the employer and employee have no leeway here—they must follow the order.
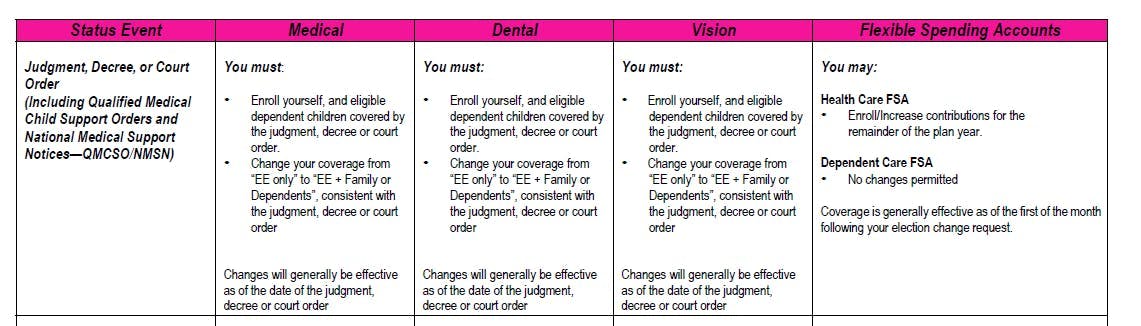
Section 125 Permitted Election Change Event
Also note that a QMCSO/NMSN creates a Section 125 permitted election change event. The employee must cover the child for the duration of the order, and he can pay for the child’s (and his) coverage on a pre-tax basis through Section 125.
Coverage Effective Date
Coverage must be effective as of the earliest date possible once the employer receives the QMCSO/NMSN. That date should in most cases be no later than the first of the month following the date that the employer receives and finishes reviewing the QMCSO/NMSN.
**Regulations: **
http://www.dol.gov/ebsa/publications/qmcso.html
**Q1-12: If an order names an employee who is not enrolled in the plan, but is eligible to enroll, can the order be a medical child support order within the meaning of the QMCSO provisions?**Yes. An employee who is eligible to enroll is a participant in the plan and thus the order is a medical child support order.
[ERISA §§ 3(7), 609(a)(1)]
**Q1-13: In the case of an employee named in a medical child support order who is not enrolled, what is the plan’s obligation?**The plan administrator must determine if the order is qualified and, if so, provide coverage to the child. If the employee is eligible to participate in the plan, the child must be covered. If, as a condition for covering his dependents, the employee must be enrolled, the plan must enroll both.
**Q1-23: When must a plan begin to provide coverage to an alternate recipient pursuant to a QMCSO?**It is the view of the Department that following a determination that an order is qualified, the alternate recipient (and the participant, if necessary) must be enrolled as of the earliest possible date following such determination. For example, if an insured plan only adds new participants or beneficiaries as of the first day of each month, that plan would be required to provide coverage to the alternate recipient as of the first day of the first month following the determination that the order is qualified. As described in Q’s 1-8 and 1-9, the State laws described in section 1908 of the Social Security Act require that when a child is enrolled in a plan pursuant to a court or administrative order, that enrollment be made without regard to open season restrictions.
Treas. Reg. §1.125-4(d):
(d) Judgment, decree, or order.
(1) Conforming election change. This paragraph (d) applies to a judgment, decree, or order order) resulting from a divorce, legal separation, annulment, or change in legal custody (including a qualified medical child support order as defined in section 609 of the Employee Retirement Income Security Act of 1974 (Public Law 93-406 (88 Stat. 829))) that requires accident or health coverage for an employee’s child or for a foster child who is a dependent of the employee. A cafeteria plan will not fail to satisfy section 125 if it—
(i) Changes the employee’s election to provide coverage for the child if the order requires coverage for the child under the employee’s plan; or
(ii) Permits the employee to make an election change to cancel coverage for the child if:
(A) The order requires the spouse, former spouse, or other individual to provide coverage for the child; and
(B) That coverage is, in fact, provided.
(2) Example. The following example illustrates the application of this paragraph (d):
Example.
(i) Employer M maintains a calendar year cafeteria plan that allows employees to elect no health coverage, employee-only coverage, employee-plus-one-dependent coverage, or family coverage. M’s employee, A, is married to B and they have one child, C. Before the beginning of the year, A elects employee-only health coverage. Employee A divorces B during the year and, pursuant to A’s divorce agreement with B, M’s health plan receives a qualified medical child support order (as defined in section 609 of the Employee Retirement Income Security Act of 1974) during the plan year. The order requires M’s health plan to cover C.
(ii) Under this paragraph (d), M’s cafeteria plan may change A’s election from employee-only health coverage to employee-plus-one-dependent coverage in order to cover C.

Karen Hooper
VP, Senior Compliance Manager
Karen Hooper, CEBS, CMS, Fellow, is a Vice President and Senior Compliance Manager working closely with the Lead Benefit Counsel in Newfront's Employee Benefits division. She works closely with internal staff and clients regarding compliance issues, providing information, education and training.